Posterior vitreous detachment is associated with an elevated occurrence of eye floaters and poses an increased risk of retinal detachment.
Have you ever wondered why paying attention to eye floaters is crucial if you or your loved one is at risk of retinal detachment? Additionally, what role does posterior vitreous detachment play in all of this? If you're curious to learn about these topics in a simple and easy-to-understand manner, you've come to the right place.
In this article, we will delve into retinal detachment, its connection with eye floaters, the symptoms to be aware of, and a brief overview of available treatment options. By the end of this article, you will have a good grasp of this serious condition and the significance of early intervention. So, let's embark on this enlightening journey together.
What is retinal detachment?
Retinal detachment occurs when the retina, the layer at the back of the eye, becomes separated from another layer called the retinal pigment epithelium. If left untreated, this condition can lead to significant vision loss. So, what are the causes and risk factors associated with retinal detachment?
In a healthy eye, there exists a small space known as the "subretinal space" between the retina layer and the retinal pigment epithelium. This space is typically closed off because the retinal pigment epithelium actively pumps fluid across the retina and into a layer called the choroid. This pumping action serves to maintain the cohesion of the layers, much like glue. Additionally, the cells in these layers possess interlocking shapes and an extracellular matrix that further promotes adhesion.
However, in cases of retinal detachment, the forces responsible for holding these layers together are disrupted. This disruption can occur when the pumping action of the retinal pigment epithelium is hindered or when there is damage to the interlocking shapes and extracellular matrix. Consequently, fluid begins to accumulate in the subretinal space, leading to retinal detachment.
Risk factors of retinal detachment
Studies have revealed that retinal detachment affects approximately 1 in 10,000 individuals each year. However, certain factors can elevate the risk of developing this condition.1,2
The risk of retinal detachment tends to increase as we age, primarily due to a condition called posterior vitreous detachment (PVD) becoming more common. Additionally, cataract surgery is believed to have an influence on vitreous liquefaction and the occurrence of PVD. The surgical procedure may accelerate the process of vitreous liquefaction, making the vitreous more watery and susceptible to detachment from the retina.3
Having severe myopia (nearsightedness) is a significant risk factor for retinal detachment. If you have myopia and your eye has an increased axial length (meaning it is longer than usual from front to back), you are more susceptible to retinal detachment.4
Furthermore, if you have experienced a retinal detachment in the past, you are more likely to have another occurrence in the future. Additionally, family history can play a role as certain traits, including increased axial length and degenerative retinal conditions, can be inherited.3,5
Other risk factors for retinal detachment include severe eye injuries and specific eye diseases such as retinoschisis (splitting of the retina), uveitis (inflammation of the uvea), or thinning of the peripheral retina (lattice degeneration). These factors can weaken the structural integrity of the retina and increase the likelihood of detachment.
Understanding the connection between eye floaters and retinal detachment
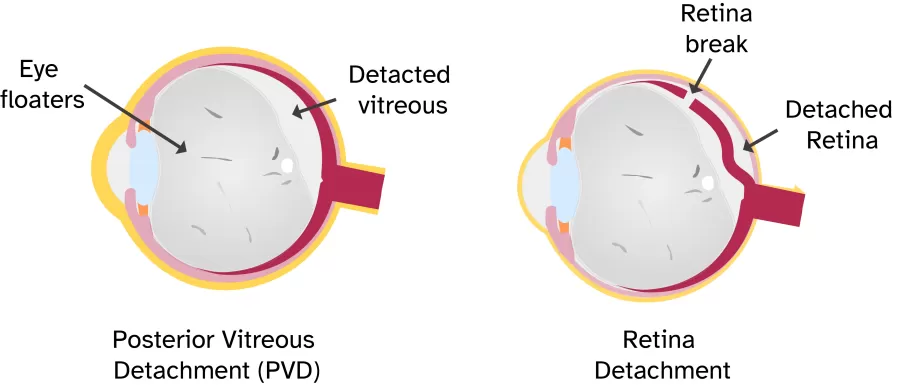
To grasp the relationship between retinal detachment and eye floaters, it's essential to first understand a condition called posterior vitreous detachment (PVD). PVD occurs when the gel-like substance called the vitreous separates from the retina, causing the floaters to become more mobile.
Eye floaters are small specks or cobweb-like shapes that sometimes appear to be floating in your field of vision. They are caused by tiny clumps of collagen fibers or cells in the gel-like substance of the eye called the vitreous. These clumps cast shadows on the back part of the eye called the retina, which is responsible for sensing light.
It's worth noting that individuals with PVD also have a higher risk of experiencing retinal breaks or tears, which can potentially progress to retinal detachment. Studies have revealed that a small percentage of the population will develop asymptomatic retinal breaks during their lifetime, but most of these breaks do not lead to detachment. However, it is important to highlight that when researchers examined patients who had reported flashes of light or floaters, they discovered that 61% of the eyes with retinal breaks eventually developed retinal detachment.
Recognizing the signs of retinal detachment
Retinal detachment doesn't cause pain, but it almost always presents warning signs before it occurs or progresses. Being aware of these symptoms can make a significant difference in preventing irreversible damage to vision. Here are the key signs to watch out for:
Sudden appearance or increase of floaters: As mentioned, floaters are those tiny specks or cobweb-like shapes that become more noticeable after experiencing posterior vitreous detachment (PVD). If you notice a sudden increase in the number of floaters you see, it could be a sign that you have developed retinal breaks or detachment.
Flashes of light: Another warning sign to be mindful of is the presence of flashes of light. Sometimes, along with these flashes, people may see black dots falling like showers. And these black dots in time may come together and form strands, cobwebs, or a cloudy haze. These descriptions suggest that there might be bleeding inside the eye due to damaged blood vessels or the release of RPE through breaks or tears.
Gradually reduced side vision: Retinal detachment can lead to a progressive loss of peripheral vision. You may notice a gradual narrowing of your visual field or a sense that you are missing objects or details on the sides.
Curtain-like shadow: One of the most distinctive symptoms of retinal detachment is the presence of a curtain-like shadow over your field of vision. This shadow may start at the edges and gradually progress towards the center. If you observe this symptom, it is crucial to seek immediate medical attention.
Blurred vision: While blurry or hazy vision can have various causes, if it occurs along with other signs of retinal detachment, you may want to have it checked as soon as possible.
Knowing when to see a doctor is paramount when it comes to retinal detachment. This condition is a medical emergency that requires immediate intervention. If you experience the signs or symptoms mentioned above, it is vital to seek medical attention without delay. Remember, timely action can potentially save your vision.
Retinal detachment surgery and recovery
When it comes to treating retinal detachment, there are a few different surgical procedures that doctors may recommend, depending on the severity of the detachment. Let's break down these treatments in simpler terms.
- Pneumatic Retinopexy: In this procedure, the doctor injects air or gas into the middle part of the eye. This helps push the detached part of the retina back against the wall of the eye, preventing fluid from going behind the retina. Over time, the fluid that had collected under the retina naturally goes away, allowing the retina to reattach itself. In some cases, you may need to keep your head in a specific position for a few days to ensure the injected air or gas stays in the right place. Eventually, the air or gas is absorbed by your body.
- Scleral Buckling: With this treatment, the doctor sews a small piece of silicone material onto the white part of the eye called the sclera, right over the area where the detachment occurred. This material creates a gentle indentation in the eye, relieving the tension caused by the gel-like substance pulling on the retina. If there are multiple tears or holes, or if the detachment is extensive, the doctor may use a larger silicone buckle that encircles the entire eye. This doesn't block your vision and is usually a permanent fixture.
- Vitrectomy: In a vitrectomy, the doctor removes the gel-like substance inside the eye called the vitreous, along with any tissue that is pulling on the retina. Then, they fill the space with either air, gas, or silicone oil to flatten the retina. Over time, the injected substance is naturally absorbed, and the vitreous space refills with the body's own fluid. If silicone oil was used, it might need to be removed in a later surgery. Sometimes, the doctor may combine vitrectomy with a scleral buckle for more effective treatment.
After surgery, your vision may take several months to improve. You may need a second surgery for successful treatment. But some people never recover all of their lost vision.
Conclusion
Retinal detachment is a serious condition that requires prompt treatment to prevent vision loss. It's important to recognize the signs, including a sudden increase in floaters, flashes of light, blurred vision, and/or curtain-like shadow. Surgical treatment options are available, and early intervention is crucial for preserving vision; but they may take several months to become evident of its impact.
Exciting advancements in research continue to shed light on potential breakthroughs in treating retinal detachment. Stay informed and engaged with the latest developments in the field.
SOCIAL MEDIA LINK:
Want to stay connected on the newest happening? Join me
Pinterest board: https://www.pinterest.com/clearsightcorner/
- Marmor MF. Mechanisms of normal retinal adhesion. In: Ryan SJ, Wilkinson CP, Schachat AP, Hinton DR, eds. Retina. St Louis: Mosby, 2006:1891-908 [Link]
- Go, Sioe Lie et al. “Genetic risk of rhegmatogenous retinal detachment: a familial aggregation study.” Archives of ophthalmology (Chicago, Ill. : 1960) vol. 123,9 (2005): 1237-41. [Link]
- Ghazi, N G, and W R Green. “Pathology and pathogenesis of retinal detachment.” Eye (London, England) vol. 16,4 (2002): 411-21. [Link]
- Akiba J. Prevalence of posterior vitreous detachment in high myopia. Ophthalmology 1993;100:1384-8. [Link]
- Kang, Hyong Kwon, and A J Luff. “Management of retinal detachment: a guide for non-ophthalmologists.” BMJ (Clinical research ed.) vol. 336,7655 (2008): 1235-40. [Link]

Comments