Not needing more treatment for wet AMD may mean the disease is inactive but not cured.
Five years ago, my dad had his last injection to treat his wet age-related macular degeneration (wet AMD). His vision had not worsened since. And his doctor said that he was doing well and didn’t show any signs of progression. He was one of the few who had long-term remission – meaning without signs or symptoms of a condition.
Wet AMD is a leading cause of vision loss in older adults in the US. The exact cause of wet AMD is not fully understood. However, what we know is that cells at the back of the eye produce an excessive amount of vascular endothelial growth factor, also known as VEGF, a growth hormone involved in wound healing and new blood vessel formation.
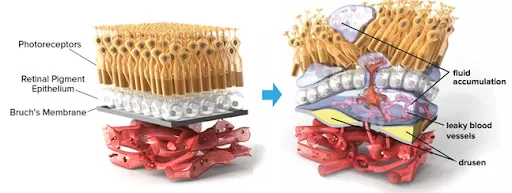
Excess VEGF is believed to cause abnormal growth of new blood vessels in the back of the eye. Since the new blood vessels are fragile, they may leak blood and fluid into the macula, damaging the retina cells and impacting vision.
The most common treatment used to treat wet AMD today is an anti-vascular endothelial growth factor (anti-VEGF). An anti-VEGF, administered as an eye injection, blocks VEGF from working and stops these blood vessels from developing.
Since wet AMD is a chronic disease, many patients need long-term anti-VEGF injections. However, a large ten-year chart review indicated that about one in ten people living with wet AMD might experience long-term remission. And, 71% of them achieved it within three years of initial treatment.
I remember that after the first few months of visiting his doctor but didn’t need to get any injections, my dad was excited and told me and the family that he was “ recovered and good now.”
He didn’t need to figure out his doctor visit schedule. He didn’t need to ask for help to drive him to the doctor. Life didn’t need to center around him managing his wet AMD. He referred to it as “his life after wet AMD”.
Wet AMD treatment with an anti-VEGF injection works by blocking VEGF and preventing the condition from worsening. It is not a cure. The condition may still spontaneously worsen.
“Patients should be counselled regarding the need for regular monitoring for early detection of recurrence, ” cautioned the leading author of the study, Dr Tiezhu Lin, Shiley Eye Institute, University of California San Diego.
In the latest Preferred Practice Pattern guidelines published by the American Academy of Ophthalmology (AAO), medical experts recommended, “patients with a high-risk AMD phenotype are at increased risk of progression to advanced AMD and should be educated about methods of detecting new symptoms of CNV [wet AMD], including self-monitoring.”
Furthermore, AAO recommends using an Amsler’s Grid every day to self-monitor for potential signs of wet AMD. Because prompt treatment can help prevent avoidable vision loss, early detection of progression with timely treatment can save sight.
Although some people may experience long-term remission, they are not cured of wet AMD. My dad learned that he is actually living with the condition. But he is happy to keep his sight on his “not-so-wet AMD.”
Want to stay connected on the newest happening? Join me
Pinterest board: https://www.pinterest.com/clearsightcorner/

Comments